Do you feel joint pains after menopause? Are your knees, hips and fingers hurting even though you don’t yet consider yourself old? The difference between those who have had knee replacements and those who haven’t. Well, maybe you’re wondering why some people get total knee replacement surgery while others don’t. If so, you are not alone. Women often want to know about joint pain after menopause, post hysterectomy pain and how hormones affect the joints. Chronic pain management expert DR. Minal chandra explains it well here.

________________________________________
Influence of Menopause and Hysterectomy on the Joints
If you are struggling with these symptoms during perimenopause, menopause or after a hysterectomy, understand that you’re not just imagining things — many other women experience the same thing. So common it is frequently ignored — pain in the joints is a symptom that occurs in 50% of women who go through menopause. There is known correlation between decreasing hormone levels and the development of joint pains. This is extensively researched in published scientific literature and can easily be managed.
When estrogen dips (whether gradually, during menopause, or suddenly, after a hysterectomy) your entire body is affected — and that includes your joints, bones and connective tissues.
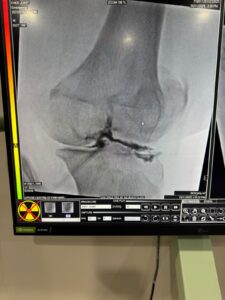
The cartilage loss fastens up, the laxity of ligaments increases your pain, inflammation increases and the other perimenopausal symptoms like mood swings, anxiety, disturbed sleep, hot flushes add to it.
This shift in hormones affects not only the reproductive system but your entire musculoskeletal architecture — something that many women are surprised to learn. Joint pain develops slowly, and many women discount it as a natural part of the aging process rather than a treatable symptom of menopause.
The big question is why do your joints act as though they are failing you during this hormonal shift — and more importantly, what can you do about it?
________________________________________
Solution: How Joint Pain Begins — Relational and Organic Reasons
The connection between hormones and joint pain is no simple quirk of nature; it results from complex biological interactions that involve your entire musculoskeletal system. Understanding these mechanisms helps to understand why women have joint pain after hysterectomy and menopause.
Estrogen has a protective function outside of reproduction. This hormone has natural anti-inflammatory properties and helps with your cartilage’s integrity and collagen production in your joints. When estrogen levels fall — whether as a result of natural menopause, or after the ovaries are removed during a hysterectomy — your joints lose that crucial cushion.
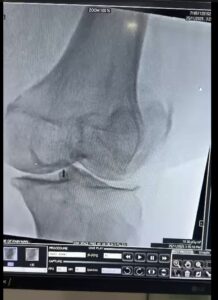
The inflammation directly stimulated by lowered estrogen levels creates the opportunity for joint problems. Studies show that post-menopausal women have higher levels of markers for inflammation, which leads to cartilage deterioration and joint stiffness. When you have less estrogen around for support, your body loses some of its capacity to repair minor joint damage.
Your body produces far less collagen during this change in hormones. This impacts not only the skin but also connective tissues within joints. The synovial fluid that helps lubricate your joints loses viscosity and you end up feeling stiffer, especially in the mornings.
Moreover, rapid hormonal fluctuations might affect sleep and stress responses, which in turn modulate pain perception and inflammation. This results in a downward spiral where lack of sleep intensifies joint pain. Breaking this vicious cycle is crucial.
________________________________________
Managing Joint Pain During Menopause
The good news is that menopause-linked joint pain doesn’t have to be your new normal. Learning how estrogen influences joint health will help point you in the direction of getting relief.
1) Lifestyle Modification – The First Step
Physical Activity
Low-Impact Cardio (3–4 times/week)
• Brisk walking – 30 min
• Cycling
• Swimming
• Reverse walking
• Aqua walking
This helps improve circulation and reduces stiffness.
Strength Training (2–3 times/week)
• Quadriceps
• Glutes
• Core strengthening
• Shoulder stabilizers
Use resistance bands or light weights. Strong muscles protect joints.
Mobility Work (Daily – 10 min)
• Gentle yoga
• Dynamic stretching
• Morning joint mobility routine
This helps reduce stiffness significantly.
________________________________________
2) Diet
You must make anti-inflammatory foods part of your daily diet. Fatty fish such as salmon, mackerel and sardines contain omega-3 fatty acids that help minimize joint inflammation. Antioxidant-rich produce like berries, leafy greens, bell peppers and cherries help fight free radicals in the joints.
Calcium and vitamin D are essential to prevent thinning of bones due to lack of estrogen. Calcium is available in dairy products, fortified plant milks and dark leafy greens. Vitamin D is available in fatty fish and fortified foods.
Cut back on inflammatory triggers such as excess sugars and refined carbohydrates. Stay hydrated — enough water ensures synovial fluid can lubricate your joints effectively.
________________________________________
3) Sleep Optimization and Stress Reduction
• At least 7–8 hours of undisturbed sleep
• Limit screen time
• Avoid alcohol and smoking
• Keep yourself hydrated
• Meditation to keep you and your hormones calm
________________________________________
Immediate Relief Strategies
Short-term remedies focus on minimizing inflammation and restoring joint function. Over-the-counter drugs such as ibuprofen may help immediate relief, but long-term management requires a comprehensive approach.
Heat therapy and mild stretching improve blood circulation and reduce morning stiffness.
________________________________________
Hormone Replacement Therapy (HRT)
Hormone replacement therapy restores estrogen in the body. Evidence suggests HRT can decrease joint pain and stiffness by 70–80% in post-menopausal women. However, HRT is not for everyone. Discuss risks and benefits with your gynaecologist.
________________________________________
Joint Health: Core Tests, Imaging and Scans
Important tests include:
• Vitamin D levels
• Inflammatory markers (CRP, ESR)
• Thyroid profile
• Rheumatoid factor (if indicated)
• DEXA scan for bone mineral density
The DEXA scan measures bone density.
T-score between -1.0 and -2.5 = Osteopenia
Below -2.5 = Osteoporosis
________________________________________
Exploring Regenerative Treatments for Joint Pain
Regenerative medicine uses the body’s healing ability to repair damaged tissue and reduce inflammation.
Platelet-rich plasma (PRP) treatment involves drawing blood, concentrating healing platelets and injecting them into the painful joint.

Stem cell therapy may help rebuild cartilage and decrease inflammation in severe cases.
Regenerative therapy advantages include:
• Natural treatment
• Same-day procedure
• No bed rest
• No mobility restriction
• Minimal downtime
Meeting your pain physician for a holistic evaluation is important.


